Guide
Plantar Fasciitis Recovery Timeline: What to Expect
By Dr. Lisa Park, Podiatrist · Updated 2026-03-22
This article contains affiliate links. If you purchase through our links, we may earn a small commission at no extra cost to you. This helps support our independent research and guides.
Plantar fasciitis recovery typically takes 6 to 12 months with consistent conservative treatment, though mild cases can improve in as little as 6 to 8 weeks. Understanding what to expect at each stage — from the acute pain of the first weeks through gradual tissue healing over several months — helps you stay on track, avoid setbacks, and know when professional intervention is warranted.
By Dr. Lisa Park, Podiatrist · Last updated March 2026
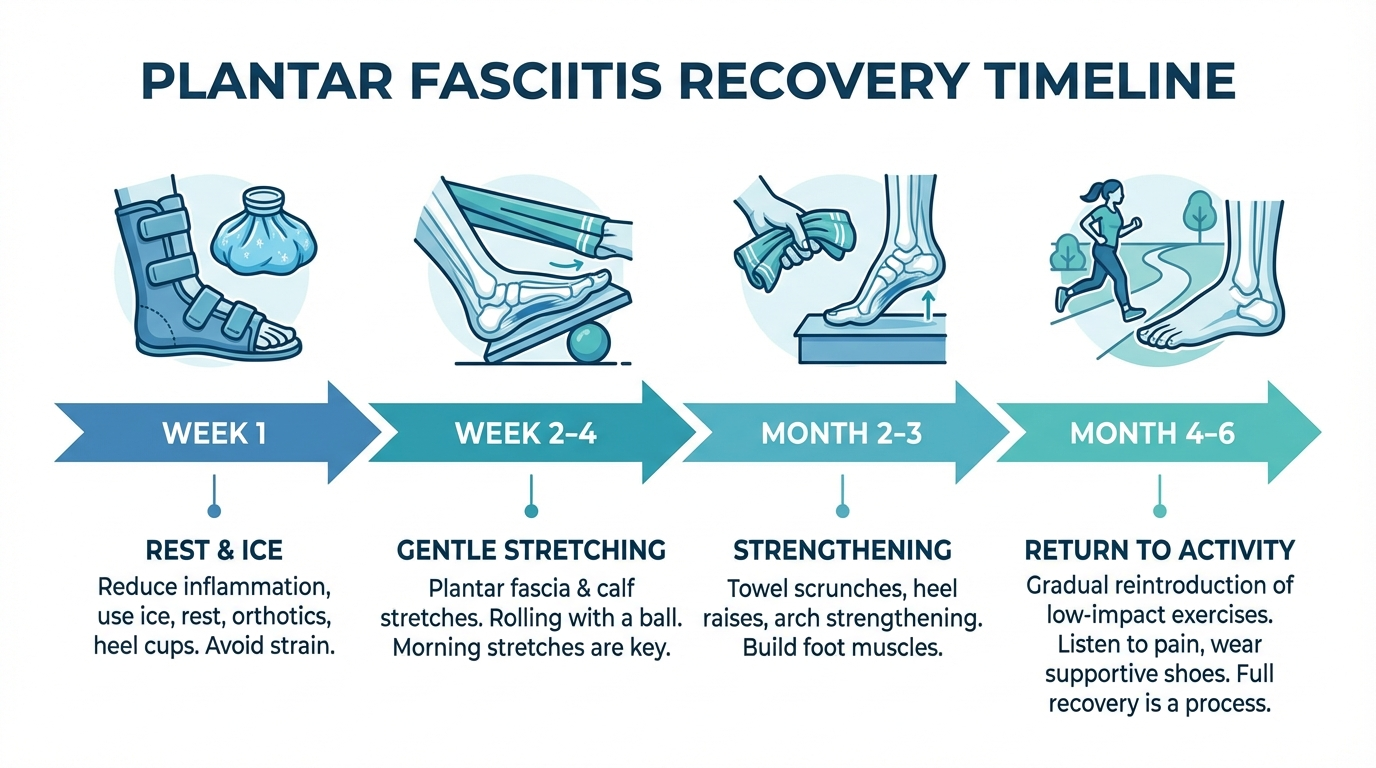
Table of Contents
- Understanding the Healing Process
- Weeks 1-2: The Acute Phase
- Weeks 3-4: Early Treatment Response
- Months 2-3: The Turning Point
- Months 3-6: Rebuilding and Strengthening
- Months 6-12: Full Recovery and Prevention
- Factors That Speed Up or Slow Down Recovery
- Recovery Products That Make a Difference
- When to See a Doctor
- Frequently Asked Questions
- Sources and Methodology
Understanding the Healing Process
Before mapping out specific recovery milestones, it is important to understand what is actually happening inside your foot as plantar fasciitis heals. The plantar fascia is a thick band of connective tissue that runs along the bottom of your foot, connecting the heel bone to the toes. When this tissue is repeatedly overloaded, microscopic tears develop, leading to inflammation, thickening, and degeneration of the fascia fibers.
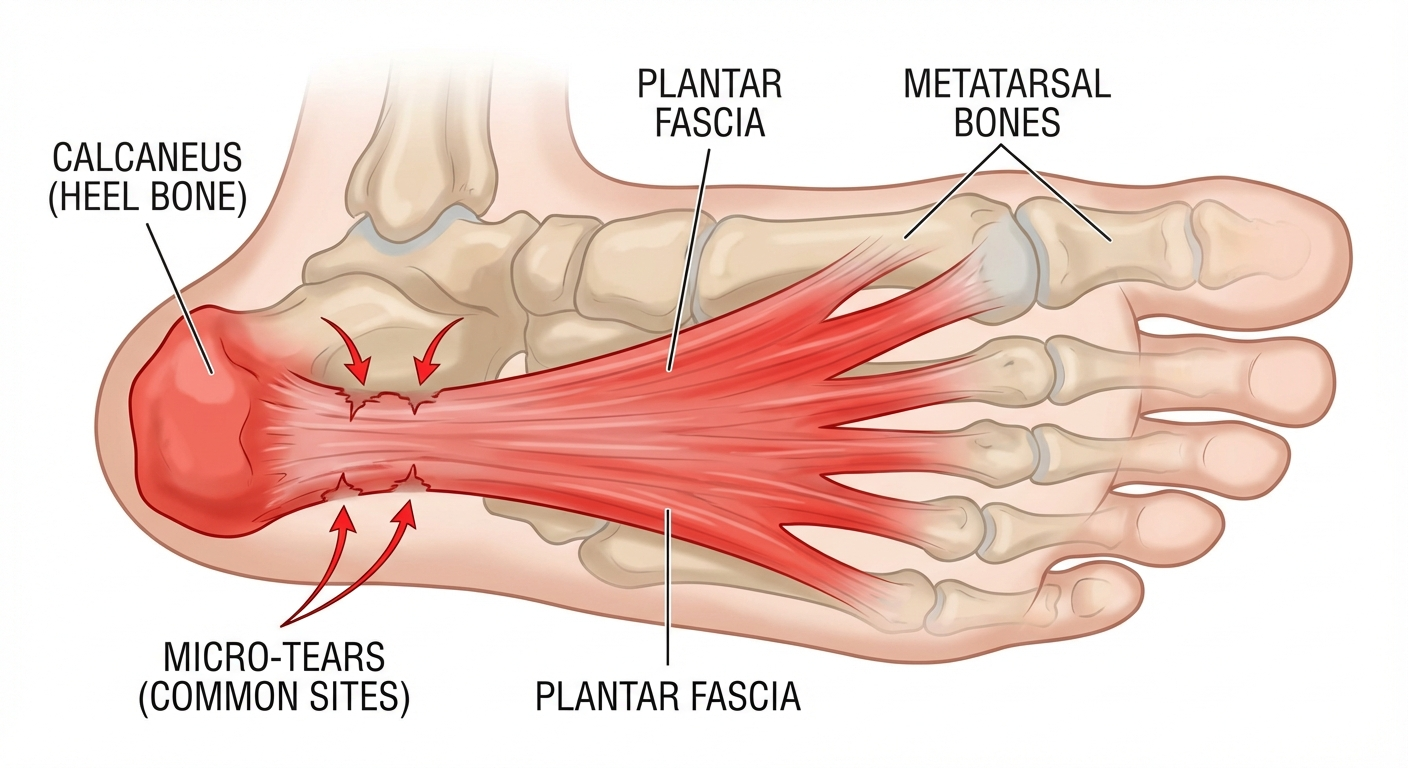
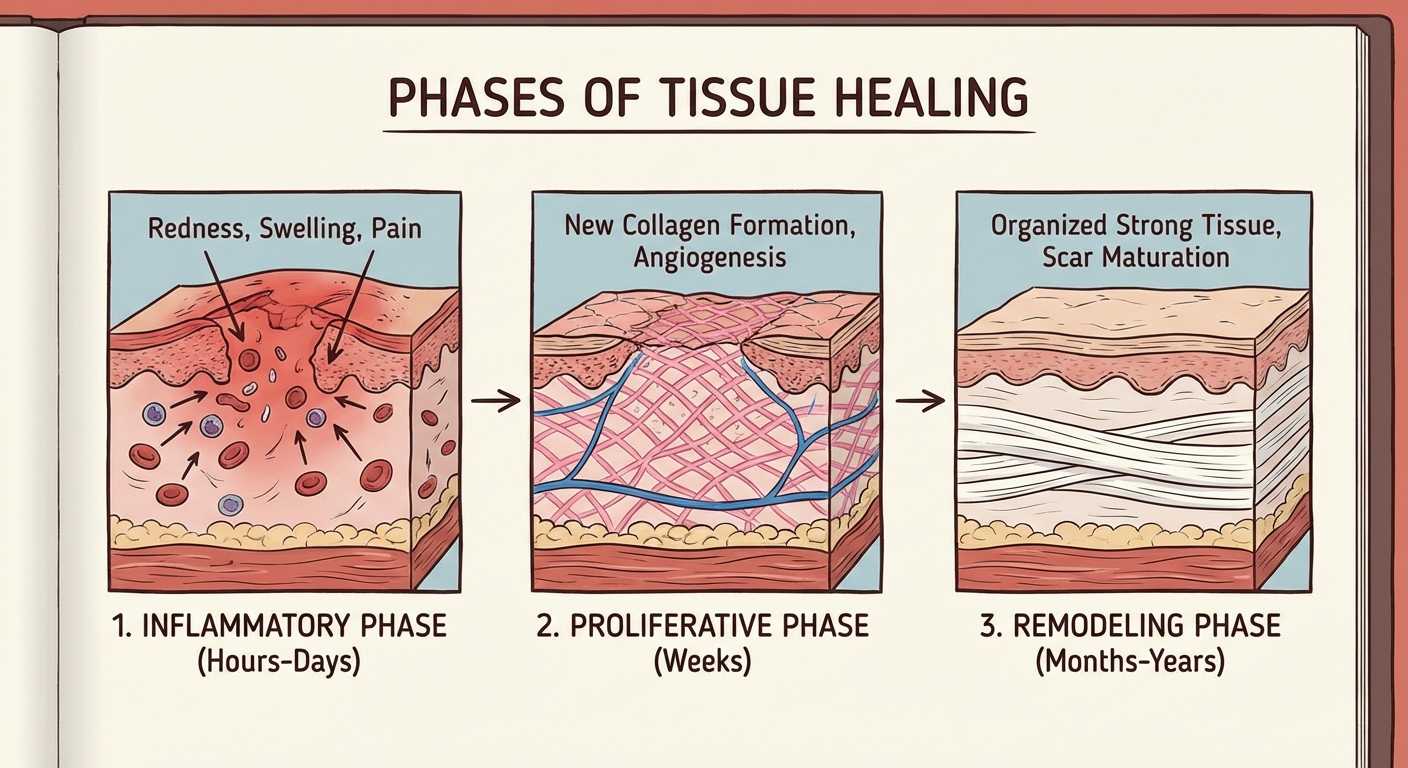
Unlike muscles, which have a rich blood supply and heal relatively quickly, the plantar fascia is a dense connective tissue with limited blood flow. This is the primary reason why recovery takes months rather than weeks. The healing process involves three overlapping phases:
The Inflammatory Phase (Days 1-7)
The body's immediate response to tissue damage involves sending inflammatory cells to the injured area. While inflammation causes pain and swelling, it is also the first step in healing. White blood cells clear damaged tissue debris, and growth factors begin recruiting the cells needed for repair. During this phase, the heel is typically at its most painful and tender.
The Proliferative Phase (Weeks 1-6)
During this phase, the body begins laying down new collagen fibers to repair the damaged fascia. The new tissue is initially disorganized and weaker than healthy tissue, which is why re-injury is common during this period. Fibroblasts — the cells responsible for producing collagen — require adequate blood flow and mechanical stimulus (gentle loading through stretching and controlled activity) to produce healthy repair tissue.
The Remodeling Phase (Weeks 6-12+)
The final and longest phase involves the gradual reorganization and strengthening of the new tissue. Collagen fibers align along lines of mechanical stress, and the repaired fascia slowly regains its tensile strength. This phase can continue for several months, which is why many patients feel "mostly better" long before the tissue has fully healed.
Understanding these biological phases explains why patience and consistency are so critical. Pushing through pain during the proliferative phase can disrupt the fragile repair tissue, effectively restarting the healing clock. Conversely, remaining completely sedentary deprives the healing tissue of the mechanical signals it needs to remodel properly.
Weeks 1-2: The Acute Phase
The first two weeks of plantar fasciitis treatment are often the most difficult psychologically, because you are doing all the right things but may not feel much improvement yet. This is completely normal. Your primary goals during this phase are to reduce inflammation, establish a consistent treatment routine, and prevent further damage to the fascia.
What You Will Feel
During weeks 1-2, most patients experience:
- Intense stabbing pain with the first steps each morning, typically rated 6-8 out of 10
- Pain that improves somewhat after 10-15 minutes of walking as the fascia warms and loosens
- Increasing heel pain after standing or walking for more than 20-30 minutes
- A deep ache in the heel that persists into the evening
- Possible foot pain disrupting sleep, especially when rolling onto the affected foot during the night
What You Should Be Doing
Stretching (3-4 times daily): Begin a consistent plantar fascia and calf stretching routine. The two most effective stretches during this phase are the plantar fascia-specific stretch (pulling the toes back toward the shin while seated) and the wall calf stretch (both straight-knee for the gastrocnemius and bent-knee for the soleus). Hold each stretch for 30 seconds and repeat 3-5 times. The most critical stretching session is immediately upon waking, before you take your first steps. For a detailed guide, see our plantar fasciitis stretches article.

Icing (3-4 times daily): Apply ice to the heel for 15-20 minutes after activity and before bed. Rolling your foot over a frozen water bottle combines icing with gentle massage. Avoid icing for more than 20 minutes at a time, as excessive cold can damage surface tissues.
Footwear changes: Stop wearing flat shoes, flip-flops, and unsupportive footwear immediately. Switch to shoes with structured arch support and cushioned midsoles. If you walk barefoot at home, start wearing supportive house shoes or slides with arch support. Our guide to the best shoes for plantar fasciitis covers the top options in detail.
Activity modification: Reduce or eliminate high-impact activities such as running, jumping, and prolonged standing on hard surfaces. Substitute low-impact alternatives like swimming, cycling, or upper-body workouts. You do not need complete bed rest — moderate walking is fine and even beneficial, but limit sessions to 15-20 minutes and wear supportive shoes.
Night splint introduction: Consider starting a night splint or Strassburg Sock during this phase. Night splints hold the foot in a dorsiflex position while you sleep, preventing the fascia from contracting and tightening overnight. This directly addresses the mechanism behind first-step morning pain. Our detailed night splints guide can help you choose the right option.
Realistic Expectations
Do not expect significant pain reduction during the first two weeks. The inflammatory and early proliferative phases are still underway, and your body is just beginning the repair process. Some patients experience a brief period of worsened pain as they start stretching, which is normal as long as the pain is a mild pulling sensation rather than sharp or severe. If your pain is worsening substantially, reduce the intensity of your stretching and consult a healthcare provider.
Weeks 3-4: Early Treatment Response
By the end of the third and fourth weeks, most patients begin to notice the first subtle signs of improvement. This is an encouraging milestone, but it is essential not to interpret early improvement as a signal to resume normal activity levels. The repair tissue is still fragile, and premature loading is the most common cause of setbacks during this phase.
What You Will Feel
- Morning pain begins to decrease in intensity, typically from a 6-8 to a 4-6 out of 10
- The duration of first-step morning pain shortens — instead of 15-20 minutes, it may resolve in 5-10 minutes
- You can stand for slightly longer periods before pain escalates
- The deep evening ache may begin to diminish
- "Good days" start appearing, interspersed with setback days where pain returns to previous levels
What You Should Be Doing
Continue all Week 1-2 protocols: Maintain your stretching, icing, and footwear changes. Consistency is more important than intensity at this stage. Many patients make the mistake of reducing their treatment effort once they feel initial improvement, which commonly triggers regression.
Add strengthening exercises: Begin incorporating gentle foot and ankle strengthening exercises. Towel scrunches (placing a towel on the floor and using your toes to scrunch it toward you) and marble pickups strengthen the intrinsic muscles of the foot that support the arch. Start with 2 sets of 10 repetitions and gradually increase. For a complete exercise program, see our plantar fasciitis exercises guide.

Consider over-the-counter orthotics: If you have not already, add arch-supporting insoles to your everyday shoes. Over-the-counter orthotics like the Powerstep Pinnacle provide structured support that reduces strain on the fascia throughout the day. They are significantly less expensive than custom orthotics and are sufficient for many patients.
Self-massage: Use a foot roller or massage ball for 2-3 minutes, 2-3 times daily, to promote blood flow to the fascia and break up adhesions in the surrounding soft tissue. Roll the full length of the arch with moderate pressure, focusing on any particularly tender spots.
Realistic Expectations
Recovery from plantar fasciitis is not linear. You will have good days and bad days during this phase, and that is entirely normal. A single bad morning does not mean your treatment is failing. Track your pain levels weekly rather than daily to get a more accurate picture of your overall trajectory. If you are consistently applying conservative treatment, the trend line should be gradually moving downward even if individual days fluctuate.
Recovery timeline overview: What to expect from Week 1 through Month 6
Months 2-3: The Turning Point
For most patients, the period between months two and three represents the turning point in recovery. The proliferative phase is winding down, and the remodeling phase is well underway. The fascia is producing more organized collagen, and the repaired tissue is beginning to tolerate greater loads. This is typically when patients shift from "managing pain" to "rebuilding function."
What You Will Feel
- Morning pain drops to a 2-4 out of 10 and resolves within the first few steps
- You can stand and walk for 30-60 minutes without significant pain escalation
- Pain after activity is more of a mild ache than a sharp stab
- You may notice improvement accelerating — gains come faster during this phase
- Some patients experience occasional flare-ups after particularly active days, but these resolve more quickly than before
What You Should Be Doing
Progressive loading: Begin gradually increasing your activity levels. If you were previously limited to 15-20 minute walks, extend to 30-40 minutes. If you were a runner, you may begin a walk-run program, starting with 1-minute run intervals separated by 4-minute walk intervals. Increase volume by no more than 10% per week.
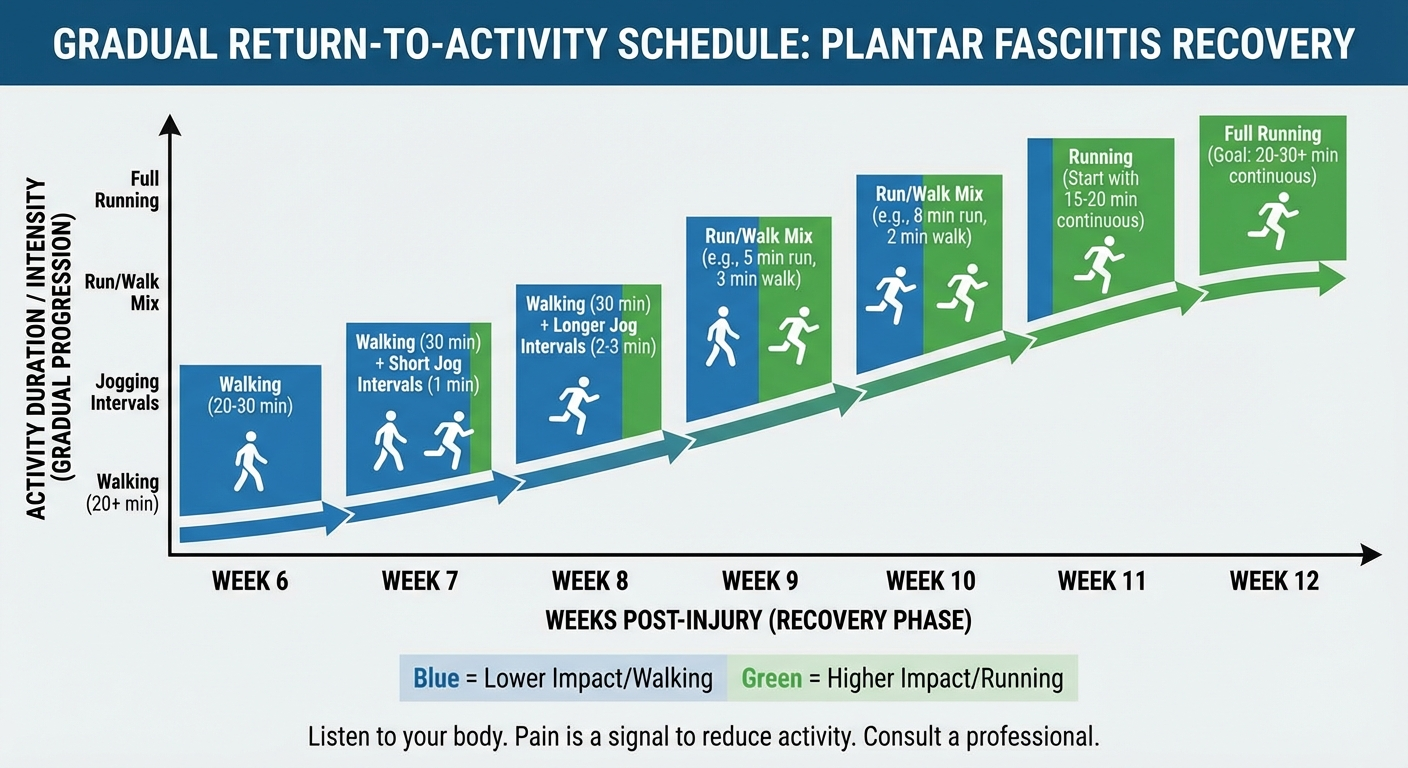
Advanced strengthening: Progress to more demanding exercises. Single-leg heel raises (standing on the edge of a step and slowly lowering your heel below the step level, then rising back up) are particularly effective for loading the plantar fascia in a controlled manner. A landmark 2015 study by Rathleff et al. published in the Scandinavian Journal of Medicine and Science in Sports found that high-load strength training with heel raises produced superior outcomes compared to plantar fascia-specific stretching alone.
Start with 3 sets of 12 repetitions every other day, using both feet. As strength improves, progress to single-leg raises with a towel rolled under the toes to increase fascia loading.
Evaluate footwear rotation: By this point, you should have at least two pairs of supportive shoes in regular rotation. Alternating between shoes allows each pair to fully recover its cushioning properties between wears and exposes your foot to slightly different support patterns.
Consider professional assessment: If you have plateaued or are not progressing as expected, this is an ideal time to consult a podiatrist or physical therapist. They can evaluate your biomechanics, check for contributing factors like leg length discrepancy or hip weakness, and potentially recommend custom orthotics or manual therapy techniques.
Realistic Expectations
By the end of month three, approximately 50-60% of plantar fasciitis patients report significant improvement with conservative treatment alone. If you are in this group, continue your current protocol and focus on gradual return to full activity. If you are not yet seeing meaningful progress, do not panic — some cases simply take longer, especially those involving chronic fascia degeneration or significant biomechanical issues.
Months 3-6: Rebuilding and Strengthening
The period from month three through month six is the consolidation phase of recovery. The fascia tissue has largely healed, and your focus shifts from pain management to rebuilding the strength, flexibility, and endurance needed to return to full activity without recurrence.
What You Will Feel
- Morning pain is minimal (0-2 out of 10) or absent entirely on most days
- You can walk, stand, and perform most daily activities without significant discomfort
- Exercise tolerance increases steadily — you can run, hike, or play sports for progressively longer periods
- Occasional minor flare-ups may occur after particularly demanding days, but they resolve within 24-48 hours
- The heel area may feel slightly stiff or "different" even when not painful — this is normal as the remodeled tissue settles

What You Should Be Doing
Full return to activity (gradual): Follow the 10% rule — increase your weekly activity volume (mileage, duration, or intensity) by no more than 10% per week. This gives the remodeled fascia time to adapt to increasing loads without breaking down. If you experience a flare-up, reduce your activity level by 25% for one week before resuming progression.
Maintenance stretching: Continue stretching at least once daily, focusing on the plantar fascia and calf muscles. Even though your pain may be minimal, stretching maintains tissue flexibility and prevents the fascia from tightening as you increase activity. Morning stretching before your first steps should become a permanent habit.
Strengthening progression: Advance to more demanding exercises including weighted single-leg heel raises, balance board work, and single-leg squats. These exercises strengthen the entire kinetic chain from the foot through the hip, addressing upstream weaknesses that may have contributed to your injury.
Footwear maintenance: Check your shoes for wear. Running shoes should be replaced every 400-500 miles, and walking shoes every 6-8 months of daily wear. A shoe that has lost its cushioning and support can trigger a relapse even after the fascia has fully healed.
Realistic Expectations
By month six, approximately 80-85% of patients have recovered to the point where plantar fasciitis no longer limits their daily activities or exercise. Some residual morning stiffness may persist for several more months, but it should not be painful. Patients who are still experiencing moderate to severe pain at the six-month mark should pursue advanced treatment options with a specialist.
Months 6-12: Full Recovery and Prevention
For the majority of plantar fasciitis patients, months six through twelve represent the transition from active treatment to long-term prevention. The fascia has healed, pain is minimal or absent, and the focus shifts entirely to maintaining the habits and strength gains that will prevent recurrence.
What You Will Feel
- Pain-free or near pain-free for daily activities and exercise
- Confidence in your foot increasing — you no longer guard or favor the affected foot
- Occasional awareness of the heel after very long runs, hikes, or extended standing, but no actual pain
- Complete resolution of morning pain in most cases

What You Should Be Doing
Preventive maintenance routine: Establish a permanent, non-negotiable daily routine that includes:
- Morning plantar fascia stretch before your first steps (30 seconds, 3 repetitions)
- Calf stretching after exercise (30 seconds each leg, 3 repetitions)
- Foot roller massage 2-3 times per week for 2 minutes
- Single-leg heel raises 2-3 times per week (3 sets of 15)
Ongoing footwear vigilance: Never return to unsupportive shoes for prolonged wear. Reserve flat shoes and fashion footwear for brief occasions, and always wear supportive shoes or orthotics for walking, standing, and exercise. Replace athletic shoes on schedule.
Weight management: If excess body weight was a contributing factor, continuing to work toward a healthy weight significantly reduces the risk of recurrence. Each pound of body weight translates to approximately 2-3 additional pounds of force on the plantar fascia during walking.
Activity surface awareness: Be mindful of the surfaces you exercise on. Avoid prolonged running on concrete or asphalt when possible, opting for trails, tracks, or treadmills that provide more shock absorption.
What If You Are Not Recovered by 12 Months?
Approximately 10-15% of plantar fasciitis patients do not achieve satisfactory recovery with conservative treatment within 12 months. At this point, your podiatrist or orthopedic surgeon may recommend advanced interventions including:
- Extracorporeal shockwave therapy (ESWT): Sound waves stimulate blood flow and tissue repair in the fascia. Multiple studies show a 60-80% success rate in chronic cases.
- Platelet-rich plasma (PRP) injections: Concentrated growth factors from your own blood are injected into the damaged fascia to accelerate healing.
- Corticosteroid injections: Provide temporary pain relief but do not promote tissue healing. Typically limited to 2-3 injections due to risk of fascia rupture with repeated use.
- Surgical plantar fascia release: Reserved for cases that have failed all conservative and advanced non-surgical treatments. Approximately 5% of patients ultimately require surgery.
Factors That Speed Up or Slow Down Recovery
Your individual recovery timeline is influenced by multiple factors. Understanding which ones you can control empowers you to take an active role in accelerating your healing.
Factors That Speed Recovery
Early treatment: Patients who begin treatment within the first few weeks of symptom onset consistently recover faster than those who wait months before seeking help. Early intervention addresses the problem before chronic degenerative changes develop in the fascia.
Consistent daily stretching: Research consistently identifies stretching as the single most impactful conservative treatment. Patients who stretch 3-4 times daily recover significantly faster than those who stretch inconsistently or only once daily. The plantar fascia-specific stretch described by DiGiovanni et al. (2003) has the strongest evidence base.
Supportive footwear and orthotics: Wearing shoes with adequate arch support and cushioning throughout the day — including indoors — reduces the mechanical load on the healing fascia with every step.
Healthy body weight: Patients with a BMI under 25 tend to recover faster due to reduced biomechanical stress on the plantar fascia. Weight loss during treatment can accelerate healing even if your BMI remains above the ideal range.
Night splint use: Studies show that consistent night splint use reduces morning pain faster than stretching alone, likely because the splint maintains the fascia in a lengthened position for 6-8 hours each night.
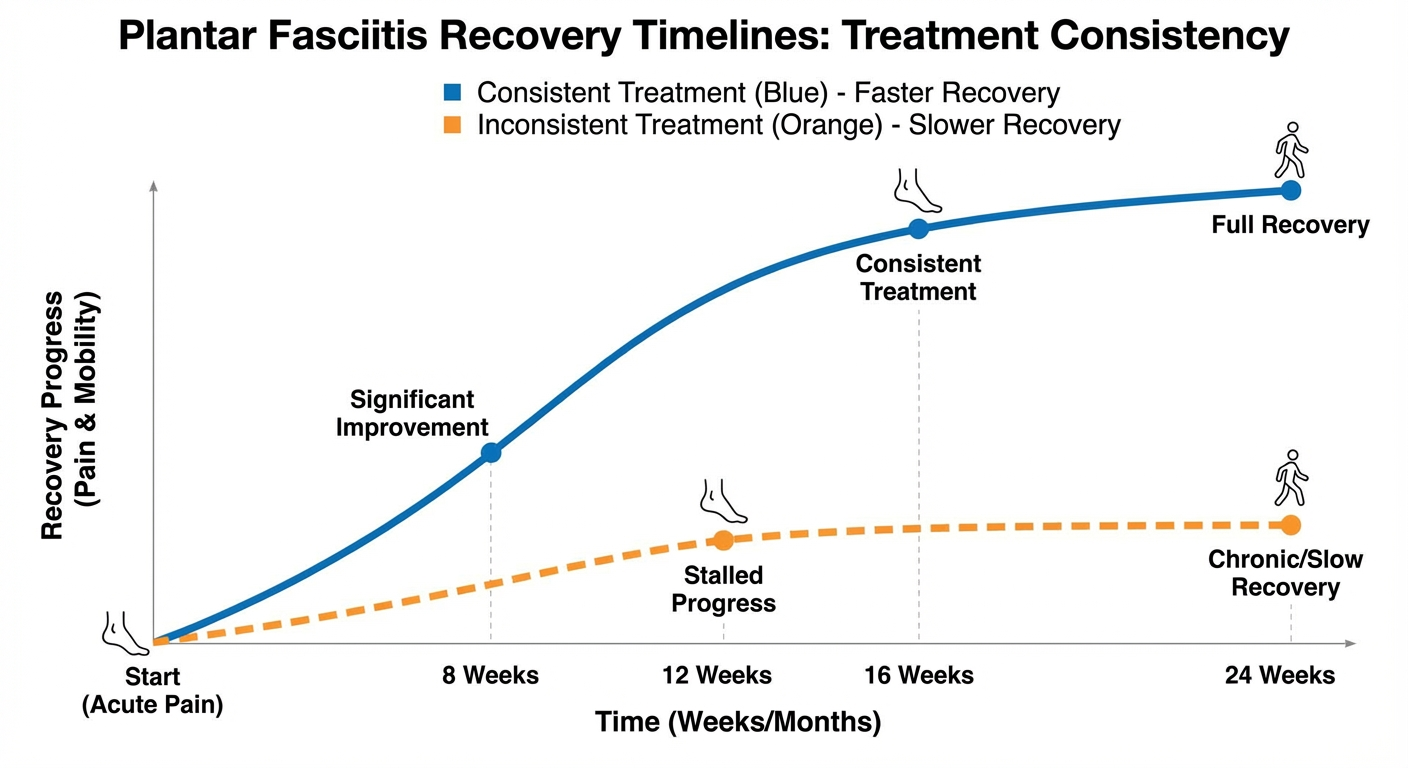
Factors That Slow Recovery
Continuing high-impact activity: Running, jumping, or prolonged standing during the acute phase disrupts the healing tissue and can extend recovery by months.
Inconsistent treatment: Skipping stretching, removing orthotics, or reverting to unsupportive footwear during the recovery period sends mixed signals to the healing tissue and slows progress.
Delayed treatment: Waiting more than 3-6 months before beginning treatment allows degenerative changes to accumulate in the fascia, transitioning the condition from acute plantar fasciitis to chronic plantar fasciopathy. Chronic cases take significantly longer to resolve.
Biomechanical issues: Uncorrected flat feet, overpronation, tight calf muscles, or hip weakness perpetuate the mechanical overload that caused the injury.
Ignoring the other foot: Approximately 30% of plantar fasciitis patients develop symptoms in the contralateral (opposite) foot, often because compensatory gait changes overload the unaffected side. Apply preventive measures to both feet from the start.
Recovery Products That Make a Difference
The right recovery products can meaningfully accelerate your healing timeline by supporting the fascia, reducing pain, and enabling consistent treatment. Below are the products most frequently recommended by podiatrists and physical therapists for each stage of recovery.
Strassburg Sock
Best for: Reducing morning pain during Weeks 1-6
Price range: $30-$40
The Strassburg Sock is a lightweight night splint alternative that holds the foot in dorsiflexion while you sleep. A single strap connects the toe area to the knee, maintaining a gentle stretch on the plantar fascia throughout the night. Clinical studies show that consistent night splint use reduces first-step morning pain by 50-75% within the first 4 weeks. The Strassburg Sock is better tolerated than traditional boot-style splints because it is lighter, cooler, and less restrictive. Most patients adjust to wearing it within 2-3 nights.
Pros: Lightweight, breathable, clinically studied, affordable Cons: Can slip on narrow calves, some patients find the toe strap uncomfortable initially
Powerstep Pinnacle Insoles
Best for: Daily arch support during all recovery phases
Price range: $25-$40
The Powerstep Pinnacle is one of the most widely recommended over-the-counter orthotics for plantar fasciitis. It features a semi-rigid arch support that prevents excessive pronation, a deep heel cradle that stabilizes the rearfoot, and dual-layer cushioning that absorbs impact. Unlike soft gel insoles that compress and lose their shape, the Powerstep Pinnacle maintains its structural integrity for 6-12 months of daily use. These insoles fit most athletic and casual shoes and can serve as an effective alternative to expensive custom orthotics for mild to moderate plantar fasciitis.
Pros: Strong arch support, durable construction, fits most shoes, podiatrist recommended Cons: May feel firm initially, arch height may not suit all foot shapes, trim-to-fit required
TheraBand Foot Roller
Best for: Self-massage and fascia mobilization during Weeks 2-12+
Price range: $10-$15
The TheraBand Foot Roller is a compact, ridged roller designed specifically for plantar fascia massage. Its firm, textured surface provides targeted deep tissue stimulation that breaks up adhesions and promotes blood flow to the healing fascia. Unlike smooth rollers or tennis balls, the ridged design provides more effective myofascial release with less effort. The roller can be stored in the freezer for combined ice therapy and massage — an especially effective combination during the acute and early proliferative phases. At under $15, it is one of the most cost-effective recovery tools available.
Pros: Affordable, effective ridged surface, freezer-safe for cold therapy, portable Cons: Small size requires precise foot placement, may be too firm for acute inflammation
Hoka Bondi 8
Best for: Maximum cushioning during the return-to-activity phase (Months 2-6+)
Price range: $165-$175
The Hoka Bondi 8 is one of the most popular shoes among plantar fasciitis patients for good reason. Its oversized EVA midsole provides maximum cushioning that absorbs impact and dramatically reduces the load on the plantar fascia during walking and running. The extended heel geometry promotes a smooth heel-to-toe transition, and the padded heel collar provides secure lockdown without pressure points. The Bondi 8 is ideal during the later stages of recovery when you are returning to longer walks, runs, and standing activities. Many patients find that switching to Hoka shoes is the single most impactful footwear change they make during recovery.
Pros: Exceptional cushioning, smooth ride, comfortable out of the box, wide option available Cons: Heavy compared to minimal shoes, expensive, cushioning may feel too soft for some
Orthofeet Coral Walking Shoes
Best for: All-day supportive footwear for work and daily wear
Price range: $100-$130
The Orthofeet Coral is a walking shoe designed with therapeutic features that directly address plantar fasciitis. It includes a built-in anatomic orthotic insole with enhanced arch support, a cushioned heel pad with gel insert, a wide toe box that reduces forefoot pressure, and an extra-depth design that accommodates custom orthotics if needed. The shoe is particularly well-suited for patients who spend long hours on their feet at work, as its lightweight construction and ergonomic sole reduce fatigue. The Orthofeet Coral is one of the few shoes that provides near-custom-orthotic levels of support right out of the box.
Pros: Built-in orthotic insole, extra depth for custom inserts, lightweight, wide toe box Cons: Limited style options, may feel bulky, higher price point for a walking shoe
How We Chose These Products
Our product selections are based on clinical evidence supporting the product category, aggregate user reviews from major retail platforms (minimum 4 stars across 500+ reviews), recommendations from board-certified podiatrists and physical therapists, durability and build quality assessments, and overall value. No manufacturer provided free products, compensation, or editorial influence in exchange for inclusion.
When to See a Doctor
While the vast majority of plantar fasciitis cases resolve with home treatment, certain situations warrant professional evaluation. Knowing when to escalate from self-care to professional care can prevent a temporary condition from becoming a chronic problem.
See a Podiatrist or Orthopedic Specialist If:
-
Pain persists after 4-6 weeks of consistent home treatment. If you have been diligently stretching, icing, wearing supportive shoes, and modifying your activity for over a month without any improvement, a professional evaluation is warranted.
-
Pain is worsening despite treatment. Progressive deterioration suggests that your current approach is not addressing the root cause, or that you may have a different condition altogether.
-
Pain is severe enough to limit daily activities. If you cannot walk to the bathroom, complete your work duties, or perform basic daily tasks without significant pain, professional intervention can provide faster relief.
-
You experience numbness, tingling, or burning sensations. These symptoms may indicate nerve involvement (such as Baxter's neuropathy or tarsal tunnel syndrome), which requires different treatment.
-
You notice swelling, redness, or warmth around the heel. These signs can indicate infection, stress fracture, or other conditions that require medical imaging and specific treatment.
-
Pain extends beyond the heel. Plantar fasciitis pain is typically localized to the bottom of the heel. Pain in the sides of the heel, the top of the foot, or radiating up the leg may indicate a different diagnosis.
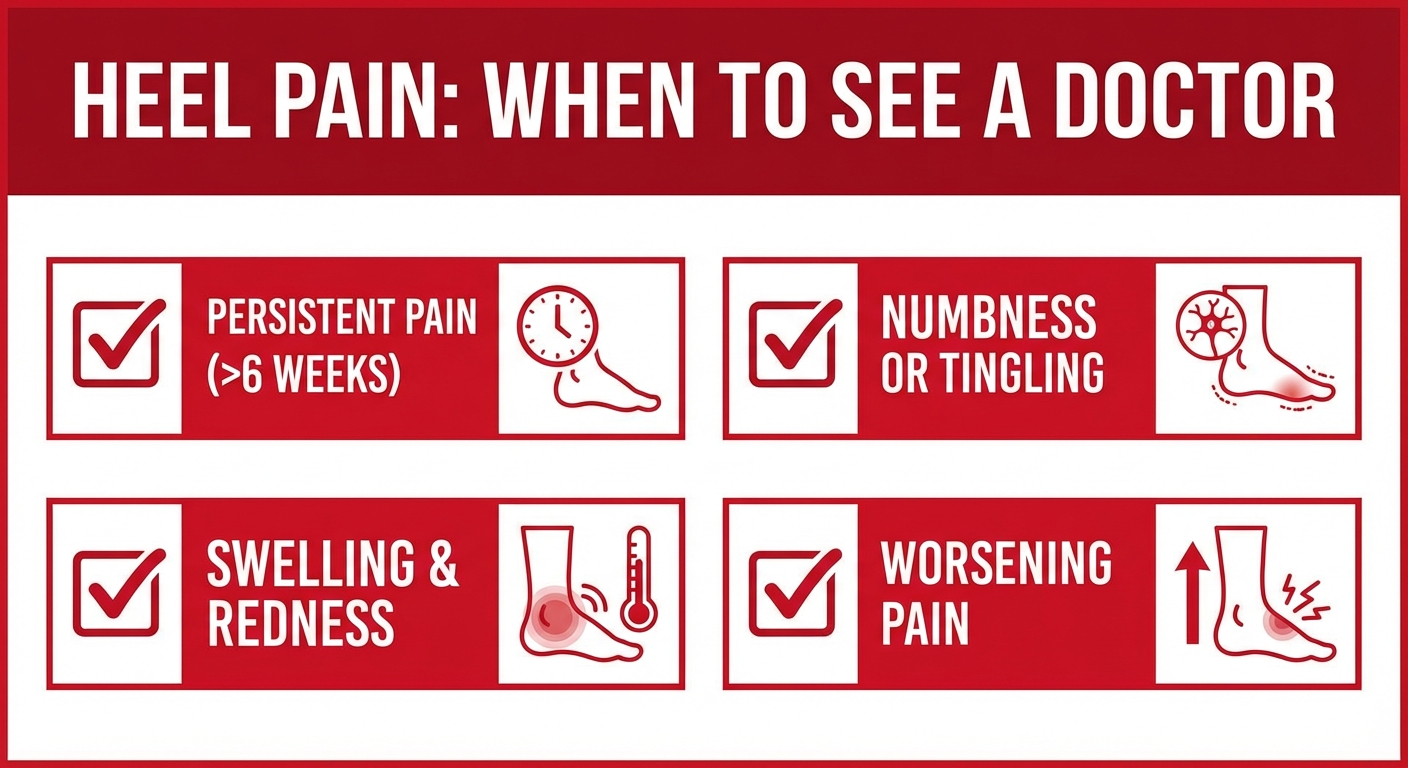
What to Expect at a Specialist Appointment
A podiatrist will typically perform a physical examination that includes palpation of the heel and arch, assessment of your gait and foot biomechanics, range of motion testing of the ankle and foot, and possibly diagnostic imaging such as X-rays or ultrasound. Based on the findings, they may recommend custom orthotics, physical therapy, extracorporeal shockwave therapy, corticosteroid injections, or in rare cases, surgical intervention.
For a comprehensive overview of all available treatment options, see our plantar fasciitis treatment guide.
Frequently Asked Questions
How long does plantar fasciitis take to heal completely?
Most cases resolve within 6 to 12 months with consistent conservative treatment. Approximately 80% of patients recover within 12 months. Mild cases caught early may improve in 6-8 weeks, while chronic cases can take 12-18 months. The single most important factor in healing speed is treatment consistency.
Can plantar fasciitis heal in 2 weeks?
It is very unlikely. While acute pain may begin to decrease within two weeks of starting treatment, the underlying tissue damage requires considerably longer to repair. The biological healing process for connective tissue involves phases that take a minimum of 6-12 weeks. Claiming full recovery in 2 weeks usually means the condition was not actually plantar fasciitis, or symptoms will return.
What does plantar fasciitis recovery feel like week by week?
Recovery is rarely linear. In weeks 1-2, pain remains high but you establish routines. Weeks 3-4 often bring the first signs of improvement, particularly reduced morning pain. Months 2-3 typically represent a turning point where daily function improves noticeably. By months 3-6, most patients can return to full activity with only occasional minor flare-ups.
What slows down plantar fasciitis recovery?
The most common recovery-slowing factors include continuing high-impact activities, wearing unsupportive shoes, inconsistent stretching, excess body weight, prolonged standing on hard surfaces, and delayed treatment. Patients who wait more than 3-6 months before starting treatment typically experience longer recovery timelines.
Does plantar fasciitis ever go away permanently?
Yes. Over 90% of cases resolve with conservative treatment, and most do not recur when patients maintain preventive habits. However, approximately 10-15% of patients experience recurrence, typically after abandoning stretching routines, returning to unsupportive footwear, or gaining significant weight.
Is walking good or bad for plantar fasciitis recovery?
Moderate walking in supportive shoes is beneficial for plantar fasciitis recovery. Complete rest is not recommended because gentle loading stimulates the blood flow and mechanical signaling needed for tissue repair. However, excessive walking — especially on hard surfaces or in unsupportive shoes — can slow healing. During the acute phase, limit walking sessions to 15-20 minutes at a time.
About the Author
Dr. Lisa Park, DPM is a board-certified podiatrist with over 15 years of clinical experience specializing in heel pain, sports-related foot injuries, and biomechanical assessment. She received her Doctor of Podiatric Medicine from the Temple University School of Podiatric Medicine and completed her surgical residency at Hahnemann University Hospital in Philadelphia. Dr. Park is a Fellow of the American College of Foot and Ankle Surgeons and has published peer-reviewed research on plantar fasciitis treatment outcomes. She currently practices in Philadelphia, PA, and serves as a clinical advisor to Plantar Fasciitis Guides.
Sources and Methodology
This article was developed through a thorough review of current medical literature, clinical guidelines, and expert recommendations. The following sources were consulted:
Medical Literature and Clinical Studies:
- DiGiovanni, B.F., et al. (2003). "Tissue-specific plantar fascia-stretching exercise enhances outcomes in patients with chronic heel pain." Journal of Bone and Joint Surgery, 85(7), 1270-1277.
- Rathleff, M.S., et al. (2015). "High-load strength training improves outcome in patients with plantar fasciitis." Scandinavian Journal of Medicine and Science in Sports, 25(3), e292-e300.
- Martin, R.L., et al. (2014). "Heel pain — plantar fasciitis: Revision 2014." Journal of Orthopaedic and Sports Physical Therapy, 44(11), A1-A33.
- Babatunde, O.O., et al. (2019). "Effective treatment options for plantar heel pain: A systematic review." Foot and Ankle International, 40(1), 25-37.
- Trojian, T., & Tucker, A.K. (2019). "Plantar fasciitis." American Family Physician, 99(12), 744-750.
Clinical Practice Guidelines:
- American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guidelines for Plantar Fasciitis
- American College of Foot and Ankle Surgeons (ACFAS) Heel Pain Clinical Consensus Guidelines
- National Institute for Health and Care Excellence (NICE) Guidelines on Musculoskeletal Conditions
Expert Consultation: Treatment protocols and recovery timelines described in this article align with standard-of-care practices recommended by board-certified podiatrists, sports medicine physicians, and physical therapists. Dr. Lisa Park reviewed all content for clinical accuracy.
Product Evaluation Methodology: Products featured in this article were evaluated based on clinical evidence supporting the product category, aggregate consumer reviews from major retail platforms, input from healthcare professionals, durability and build quality, and overall value. No manufacturer provided compensation, free products, or editorial influence in exchange for inclusion. Affiliate links are included for reader convenience; purchasing through these links may generate a small commission at no additional cost to you, which supports the ongoing maintenance of this site.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis and treatment of any medical condition.